This page provides information and resources on emerging or communicable diseases highlighted by the Public Health Department. Click the links above for more information about communicable diseases.
H5N1 risk to general population: Low
Human Cases in Illinois: 0
Latest guidance on H5N1:
- Do not handle wild birds, whether live or deceased
- Avoid contact with bird feces
- Do not attempt to capture birds displaying signs of illness
- Keep your dogs and other pets away from deceased birds
- If you have backyard chickens, click to read the guidance from the CDC.
- Avoid drinking raw milk
See the full list of protective actions from the CDC.
What is H5N1
H5N1 is also known as “highly pathogenic avian influenza (HPAI) A(H5N1)” or bird flu. It is a virus that originated in wild birds, and has spread to commercial and domesticated poultry. Recently, it has also spread to other domesticated animals and dairy cows.
Why are experts concerned?
Bird flu viruses do not normally infect humans, however, there have been human cases confirmed by the CDC across the country. See the latest numbers here: CDC H5N1 Dashboard.
Since the spring of 2024, sporadic human infections have been reported in the United States, associated with poultry or dairy cattle exposures. There are ongoing multi-state outbreaks of H5N1 virus among dairy cattle and poultry.
Populations currently most at risk for contracting H5N1
Signs and symptoms of H5N1
CDC current situation report
Click the sections below for information from the Public Health Department related to COVID-19. For more information, contact 708.358.5410 or health@oak-park.us.
Free COVID-19 tests
Free COVID-19 Tests will be available at the end of September 2024. U.S. households will be eligible to order 4 free COVID-19 tests at COVIDTests.gov. The COVID-19 Tests will detect current COVID-19 variants and can be used through the end of the year.
COVID-19 testing can help you know if you have COVID-19 so you can decide what to do next, like getting treatment to reduce your risk of severe illness and taking steps to lower your chances of spreading the virus to others.
Visit COVIDtests.gov for updates on this program and to order your tests when they become available.
COVID-19 test expiration dates
Many COVID-19 tests have extended expiration dates. If you think your COVID-19 test may have expired, check the FDA’s website for information on authorized at-home test diagnostic tests and expiration dates.
COVID-19 Vaccine
CDC recommends everyone ages 6 months and older receive an updated 2024-2025 COVID-19 vaccine to protect against the potentially serious outcomes of COVID-19 this fall and winter whether or not they have ever previously been vaccinated with a COVID-19 vaccine. Data continue to show the importance of vaccination to protect against severe outcomes of COVID-19 and flu, including hospitalization and death. To learn more about the current vaccines, visit the CDC's COVID-19 webpage.
Where to find the COVID-19 vaccine in Oak Park
Homebound Senior Citizens, Insured and Uninsured
- Call AgeOptions at 708.383.0258 to request a COVID-19 vaccine.
Insured Individuals
- Call your physician and make an appointment. Some doctor’s offices do not have the COVID-19 vaccine in stock yet but will soon.
- Walgreens, CVS, Jewel Osco will all have appointments available soon for people 4 years old and older.
Uninsured Individuals
Call the Cook County Department of Public Health Clinic in North Riverside (1800 S. Harlem Avenue) at 312.864.0200 and make an appointment.
As of June 10, 2024, there were 52 confirmed and 19 probable Mpox cases in Chicago and Cook County. An overwhelming majority - 98% - of Mpox cases this year have occurred in males, with nearly half of those infected between the ages of 25 and 34. While most cases result in mild illness, six people required hospitalization due to their condition.
With summer arriving, the CDC anticipates cases may continue rising significantly in July and August when warmer temperatures and more social gatherings could further spread the virus. See below for vaccine recommendations, signs, symptoms, and how to prevent the spread of Mpox.
Mpox vaccine information
There is a vaccine available to prevent the spread of mpox(PDF, 174KB) . Currently, CDC does not recommend routine immunization against mpox for the general public.
Mpox vaccination should be offered to people with high potential for exposure to mpox:
- People who had known or suspected exposure to someone with mpox.
- People who had a sex partner in the past 2 weeks who was diagnosed with mpox.
- Gay, bisexual, and other MSM, and transgender or nonbinary people (including adolescents who fall into any of these categories) who, in the past 6 months, have had
- A new diagnosis of one or more sexually transmitted diseases (e.g., chlamydia, gonorrhea, syphilis).
- More than one sex partner
- People who have had any of the following in the past 6 months
- Sex at a commercial sex venue
- Sex in association with a large public event in a geographic area where mpox transmission is occurring.
- Sex in exchange for money or other items
- People who are sex partners of people with the above risks
- People who anticipate experiencing any of the above scenarios
- People with HIV infection or other causes of immunosuppression who have had recent or anticipate potential mpox exposure
- People who work in settings where they may be exposed to mpox
- People who work with orthopoxviruses in a laboratory
If you are interested in getting a vaccination, contact the Health Department at 708.358.5480 or email health@oak-park.us.
Signs and symptoms
Most people with mpox will get a rash.
- The rash may be located in areas like the hands, feet, chest, face, on or near the genitals or anus
- The rash will go through several stages, including scabs, before healing.
- The rash can look like pimples or blisters and may be painful or itchy.
- The rash may also be inside the body, including the mouth, vagina, or anus
Images of an Mpox Rash
Content note: some of the pictures could be considered graphic by some.
Some people have developed a rash before (or without) flu-like symptoms.
- The flu-like symptoms may include fever, headache, muscle aches and backache, sore throat, cough, swollen lymph nodes, chills, or exhaustion.
- If someone has flu-like symptoms, they will usually develop a rash 1-4 days later.
Mpox symptoms usually start within 3 weeks of exposure to the virus.
The illness typically lasts 2-4 weeks. Sometimes, people get a rash first, followed by other symptoms. Others only experience a rash.
How mpox spreads
At this time, mpox is spreading mostly through close, intimate contact with someone who has the virus.
The virus can spread from person-to-person through direct contact with the infectious rash, scabs, or body fluids. It also can be spread by respiratory secretions during prolonged, face-to-face contact, or during intimate physical contact, such as kissing, cuddling, or sex. In addition, pregnant people can spread the virus to their fetus through the placenta.
Touching items (such as clothing or linens) that previously touched the infectious rash or body fluids is another way mpox spreads.
People who do not have mpox symptoms cannot spread the virus to others.
Mpox can spread from the time symptoms start until the rash has fully healed and a fresh layer of skin has formed.
Preventing the spread
- Avoid close, skin- to- skin contact with people who have a rash that looks like mpox.
- Do not touch the rash or scabs of a person with mpox.
- Do not kiss, hug, cuddle or have sex with someone with mpox.
- Do not share eating utensils or cups with a person with mpox.
- Do not handle or touch the bedding, towels, or clothing of a person with mpox.
- Wash your hands often with soap and water or use an alcohol-based hand sanitizer.
What to do if you get sick
- Isolate at home
- If you have an active rash or other symptoms, stay in a separate room or area away from people or pets you live with, when possible.
- The CDC recommends vaccination for people who have been exposed to MPV and people who are at higher risk of being exposed to mpox.
2022 Local mpox status reports
Beginning in May 2022, health organizations across the globe, including the Centers for Disease Control and Prevention, began tracking cases of Monkeypox virus (mpox), which began to spread across several countries that don't normally report cases. In August of 2022, the U.S. Department of Health and Human Services (HHS) declared a Public Health Emergency regarding mpox in order to strengthen and accelerate the response from the public health sector. The Oak Park Health Department began to accept calls related to MPV that month, between August 2022 and January 2023, the department investigated 8 potential cases. These investigations led to 22 people being vaccinated against mpox. In December of 2022, HHS said that it would not renew the declaration of the public health emergency when it expires January 31, 2023.
See below for the status reports produced by the Health Department during this public health emergency on the Village of Oak Park's operational activities in response to MPV that were issued to the Village Board as necessary. Click on the titles below to view the report:
- February 3, 2023(PDF, 138KB)
- December 30, 2022(PDF, 136KB)
- December 2, 2022(PDF, 134KB)
- November 18, 2022(PDF, 134KB)
- November 11, 2022(PDF, 133KB)
- November 4, 2022(PDF, 133KB)
- October 28, 2022(PDF, 109KB)
- October 21, 2022(PDF, 109KB)
- October 14, 2022(PDF, 108KB)
- October 7, 2022(PDF, 108KB)
- September 30, 2022(PDF, 115KB)
- September 23, 2022(PDF, 85KB)
- September 16, 2022(PDF, 84KB)
- September 9, 2022(PDF, 90KB)
- September 2, 2022(PDF, 83KB)
- August 26, 2022(PDF, 82KB)
- August 19, 2022(PDF, 81KB)
As of June 3, 2024, the Illinois Department of Public Health (IDPH) announced that the 2024 measles outbreak – the largest outbreak to affect the state of Illinois since 1990 – was officially contained. During the outbreak, which began March 7, a total of 67 measles cases were reported. A majority of cases were linked to a Chicago shelter. Cases eventually extended beyond Chicago to suburban Cook County, DuPage, Lake and Will counties, but were rapidly contained in all these other locations. No cases were ever confirmed in Oak Park. During the outbreak, the Oak Park Public Health Department hosted measles vaccine clinics at shelters for people seeking asylum from Venezuela and other Central and South American countries. The department also made the MMR (measles, mumps, rubella) vaccine available to Oak Park residents unsure of their measles vaccination status or those that wanted a booster dose due to waning immunity.
How it spreads
Measles is very contagious and spreads through the air when an infected person coughs or sneezes. If other people breathe the contaminated air or touch the infected surface, then touch their eyes, noses, or mouths, they can become infected. Someone can contract measles just by being in a room where a person with measles has been, even up to 2 hours after that person has left.
Measles is so contagious that if one person has it, up to 90% of the people close to that person who are not immune will also become infected.
People with measles can spread this disease to others four days before they have a measles rash and for four days after the rash appears. Someone who has not had the measles-mumps-rubella (MMR vaccine) or a prior infection is highly likely to get measles if they are exposed to the measles virus.
Preventing the spread and protecting yourself
As with all communicable diseases, protecting yourself against measles also protects your household and community by slowing or stopping the spread.
Vaccination
The MMR vaccine provides the best and strongest protection against this disease, and most people receive the vaccine as a child as part of the routine and recommended vaccine schedule.
If you do not know your measles immunization status, please talk to your health care provider as a simple blood test can confirm immunity.
If you or anyone in your household needs a measles vaccine, please reach out to your health care provider or pharmacy. If you need any assistance locating a vaccine, please call the Oak Park Public Health Department at 708.358.5480 or health@oak-park.us.
Some people should not get the MMR vaccine or should wait to do so. Speak with your provider before getting the vaccine if:
- You have ever had a life-threatening allergic reaction after a dose of MMR vaccine, or have a severe allergy to any part of this vaccine.
- Are pregnant or may be pregnant. Pregnant people should wait until after pregnancy to receive the MMR vaccine.
- You have a weakened immune system due to disease (such as cancer or HIV) or medical treatments (such as radiation, steroids or chemotherapy)
- Have gotten other vaccines in the past four weeks. Live vaccines given too close together might not work as well.
- You are ill. Mild illness like a cold typically is not a reason to postpone vaccination, but with moderate or severe illness, it’s best to wait. Your health care provider can advise you.
Other ways to protect yourself
If you are unsure of your immunization status or spend time in a higher-risk environment, such as a health care setting, congregate living facility or shelter, there are additional measures you can take to protect yourself. These include:
- frequent, proper handwashing with soap and warm water for at least 20 seconds
- wearing a well-fitted KN95 or N95 mask
Signs and symptoms
Measles typically starts with cough, runny nose, red eyes, and a fever that can get very high. Three to five days after these symptoms begin, a rash will begin to develop. The rash looks like tiny, red spots that start at the head and spread down to the rest of the body. If you think you or your child might have measles, call your healthcare provider immediately.
Because measles is rare due to high vaccination rates in the United States, most people have not seen a measles rash. To see images of a measles rash, click this link from the CDC (the photos will not appear immediately when the link is clicked, you will need to click a second link to see the images)
What to do if you have symptoms or are sick
Call your healthcare provider immediately if you think you or your child have been exposed to measles. Measles can be dangerous, especially for babies, young children and pregnant women.
In December of 2023, health officials noted an increase of Varicella (chicken pox) cases in Oak Park, as well as the Chicago area. Most children and adults in Illinois are expected to be protected against varicella infections either by vaccination or previous disease. The course of illness is usually mild and not life-threatening to healthy children, but it may be severe in infants, adults, and persons with compromised immune systems. In some cases, chickenpox may cause more serious illness, and may even lead to death.
See below for signs and symptoms, incubation and communicability periods, how to prevent the spread and other information.
How varicella (chicken pox) spreads
Chickenpox is one of the most readily communicable diseases. This virus can spread from person to person by direct contact with fluid from the blisters/pox, secretions from the respiratory tract, or by handling an infected person's clothing or bedding. Airborne transmission is possible through sneezing and coughing.
Incubation period and contagiousness
The incubation period (the time it takes for an infection to develop after a person has been exposed to a disease-causing organism) can be 10-21 days. The disease may be transmitted one to two days before onset of rash through the first four to five days, or until all lesions have formed crusts.
Signs and symptoms
Varicella infections do not usually cause serious illness, although they often cause children to miss days of school while they have a rash, and parents to miss work when they stay home to take care of their children.
Symptoms of varicella appear most commonly within two weeks following exposure, but may take as long as 21 days. Symptoms include:
- fever
- fatigue/a feeling of tiredness
- an itchy rash. The rash--or the pox--generally starts as little red spots on the chest, stomach or back and then on the face. The infected person may get only a few spots or a cluster of spots, or he or she may develop hundreds of spots during the first three to five days of the rash. The spots change into clear blisters filled with fluid. These blisters become cloudy, can break open and form a crust or scab in two to four days. The scabs can be very itchy.
Controlling the spread
School and public health rules require that children and adults with chickenpox be excluded from school or work for at least five days following the onset of their pox and all chickenpox are dried or crusted over. Any clothing or bedding with discharge from a patient’s discharges from the nose, throat and lesions should be disinfected.
What to do if you have symptoms or are sick
Since chickenpox has been introduced into the Oak Park area, be watchful for any symptoms. If you or your child or anyone in your household has or develops symptoms that look like chickenpox:
- Contact your regular health care provider to discuss the symptoms and to see if anyone in the home needs to be vaccinated.
- Until the symptoms resolve, avoid contact with others who have not had chickenpox or who are not vaccinated against chickenpox.
- Do not attend school, day care, work, parties and/or other gatherings until the blisters become crusted, and no new lesions appear within a 24-hours period.
- Keep all chickenpox spots and blisters and other wounds clean and watch for possible signs of infection; including increasing redness, swelling, drainage and pain at the wound site.
- If you or anyone else in your household has a weakened immune system or is pregnant and has never had chickenpox or the vaccine, talk with your doctor immediately.
Vaccination
A vaccine that can prevent chickenpox (varicella vaccine) is available and has been shown to be safe for children who are older than 12 months of age. If you or your child does not have a history of varicella (chickenpox) disease or vaccination, please consult the Oak Park Public Health Department at 708.358.5480 or your physician about acquiring vaccination.
If you or your physician have any further questions, please call the Oak Park Department of Public Health at 708.358.5480 or email heatlh@oak-park.us
Flu is a contagious respiratory illness caused by influenza viruses that infect the nose, throat, and sometimes the lungs. It can cause mild to severe illness, and at times can lead to death. The best way to prevent flu is by getting a flu vaccine each year.
How Flu Spreads
Most experts believe that flu viruses spread mainly by tiny droplets made when people with flu cough, sneeze, or talk. These droplets can land in the mouths or noses of people who are nearby. Less often, a person might get flu by touching a surface or object that has flu virus on it and then touching their own mouth, nose or possibly their eyes.
People at Higher Risk for Severe Outcomes as a Result of Flu
Anyone can get flu (even healthy people), and serious problems related to flu can happen at any age, but some people are at higher risk of developing serious flu-related complications if they get sick. This includes people 65 years and older, people of any age with certain chronic medical conditions (such as asthma, diabetes, or heart disease), pregnant people, and children younger than 5 years.
Preventing Seasonal Flu
The first and most important step in preventing flu is to get a flu vaccine each year. Flu vaccine has been shown to reduce flu related illnesses and the risk of serious flu complications that can result in hospitalization or even death. CDC also recommends everyday preventive actions (like staying away from people who are sick, covering coughs and sneezes, and frequent handwashing) to help slow the spread of germs that cause respiratory (nose, throat, and lungs) illnesses, like flu.
Below are a few graphs showing a cluster of flu cases and hospitalizations around the months of November and December, which is typical "flu season" because people tend to find themselves indoor more frequently. There are notably more cases this fall compared to last fall.
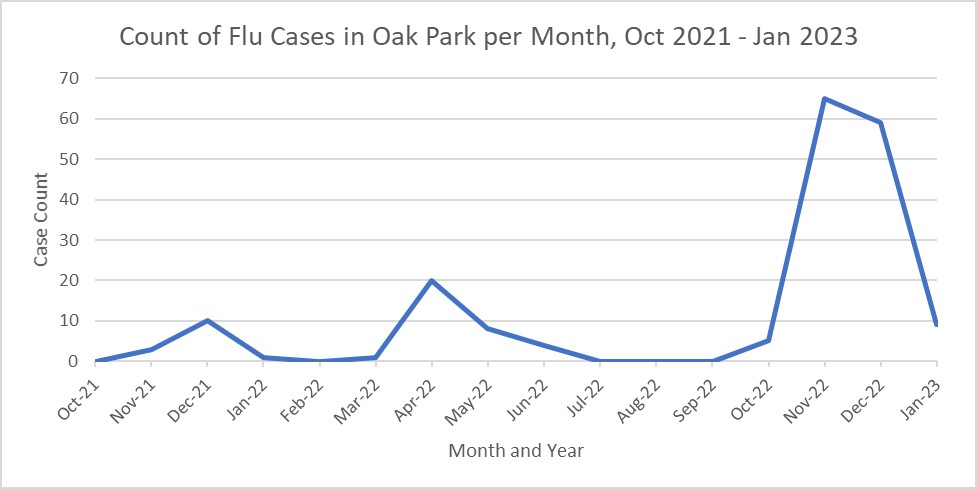
In the U.S., most flu activity starts in October and ends in May. Peak flu season is typically between December and March. Comparing our current flu season to last year's, there is a greater number of cases this season so far. The Oak Park Health Department continues to encourage flu vaccination and other behaviors to minimize the spread of the flu, including staying home when sick and frequent handwashing.
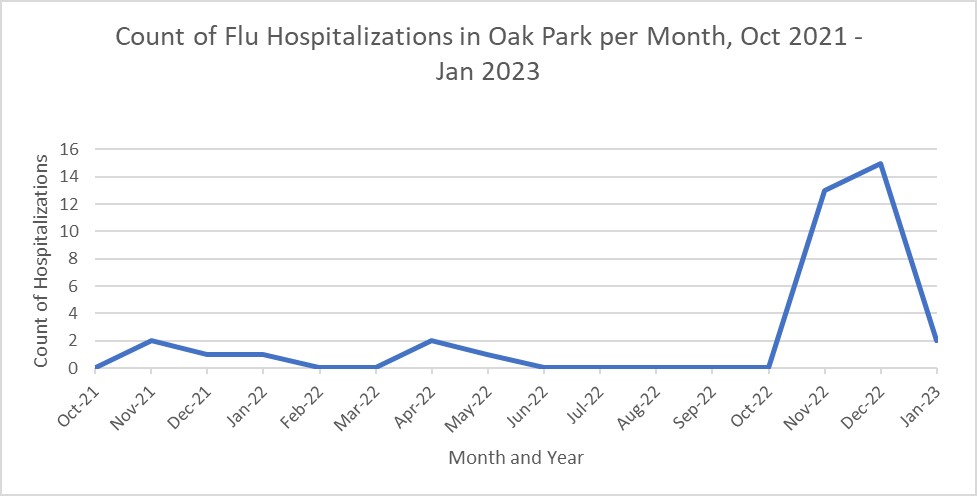
As illustrated in the graph above, this year's flu cases have been more severe and resulted in an increase in hospitalizations. Taking the precautions listed above can help protect populations more vulnerable to severe cases that require hospitalization.
In September 2022, an outbreak of Ebola was identified in Uganda. At this time, there are no cases of Ebola in the United States and Ebola does not pose a great health risk to the people of Oak Park. Since late September, the U.S. Centers for Disease Control and Prevention (CDC) and Customs and Border Protection (CBP) have been screening travelers at major airports, including O'Hare, who have been in countries most affected by the Ebola outbreak, which is primarily Uganda.
The Oak Park Health Department is monitoring the situation and will notify the public should there be any cause for action. Below is more information about the Ebola virus.
What is Ebola, signs and symptoms
What is Ebola?
Ebola is a severe disease that is caused by the Ebola virus.
What are the signs and symptoms of Ebola?
Symptoms may appear anywhere from two to 21 days after contact with the virus. Most people will begin to experience symptoms within eight to 10 days. The course of the illness typically progresses from "dry" symptoms initially (such as fever, aches and pains, and fatigue), and then progresses to "wet" symptoms (such as diarrhea and vomiting) as the person becomes sicker.
How does Ebola spread?
Ebola is spread through direct contact with blood or body fluids of a person who is sick with Ebola, or a person who has recently died from Ebola.
What are "body fluids"?
Examples include:
- urine
- saliva
- sweat
- feces
- vomit
- semen
What is "direct contact"?
This means that body fluids, such as those listed above, from an infected person (alive or dead) have touched someone's eyes, nose, mouth or an open cut, wound or abrasion.
Ebola can also be spread on objects or surfaces contaminated with blood or body fluids of an infected person.
A person who is NOT experiencing symptoms, such as fever, vomiting or diarrhea, cannot transmit the virus. Ebola is NOT spread through the air, water or food.
How long does Ebola live outside the body?
Ebola is killed with hospital-grade disinfectants such as household bleach. Ebola on dried surfaces, such as doorknobs and countertops, can survive for several hours; however, virus in body fluids (such as blood) can survive up to several days at room temperature.